
Plavix® is often prescribed as a result of coronary artery disease, as a result of periphery artery occlusive disease (obstruction of the arteries as a result of atherosclerosis or thrombus formation,) or as a result of cerebrovascular disease (damage to the blood vessels in the brain resulting in a stroke.) Antiplatelet drugs such as Plavix® have been shown to decrease morbid events in those patients with established cardiovascular disease, indicating that platelets play a considerable role in these events. Plavix® should not be administered to patients who have a stomach ulcer or those who have a condition that causes bleeding.
Ticlopidine (Ticlid®) is an older drug launched in 1979 which also acts to inhibit platelet aggregation induced by adenosine diphosphate, though it has not been as successful as clopidogrel.

Clopidogrel selectively inhibits the binding of adenosine diphosphate (ADP) to its platelet receptor PY212 and the subsequent ADP-mediated activation of the glycoprotein GPIIb/IIIa complex, thereby inhibiting platelet aggregation. Biotransformation of clopidogrel is necessary to produce inhibition of platelet aggregation,
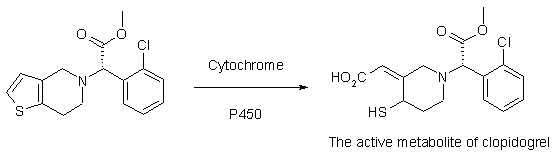
The active metabolite responsible for the activity of the drug was not isolated until 1999. Clopidogrel also inhibits platelet aggregation induced by chemicals other than ADP through blocking the amplification of platelet activation caused by the release of ADP.
Clopidogrel acts to irreversibly modify the platelet ADP receptor. As a result, platelets exposed to clopidogrel are affected for the remainder of their lifespan.
Inhibition of platelet aggregation can be seen 2 hours after a single oral dose of Plavix® . Repeated doses of 75 mg Plavix® per day inhibit ADP-induced platelet aggregation on the first day, and inhibition reaches a steady state between Day 3 and Day 7. At steady state, the average inhibition level observed with a dose of 75 mg Plavix® per day was between 40% and 60%. The aggregation of platelets and bleeding time gradually return to their baseline values after treatment is stopped, and this generally occurs in about 5 days.
Adding clopidogrel to aspirin for the use in emergency heart attack treatment could save thousands of lives according to the American College of Cardiology conference. Dr Zhengming Chen suggests that "adding 75 mg of oral clopidogrel daily to aspirin significantly reduced the relative risk of death in hospital by 7% and the risk of death, repeat heart attack or stroke by about 10%, without any significant increase in serious bleeds. These benefits were additional to those of standard heart attack treatments, and were seen even in older patients and those presenting several hours after the onset of symptoms." The result of this could be that adding clopidogrel to current therapies could benefit 1 in every 100 patients.
Clopidogrel is also more effective than aspirin in preventing heart attacks and strokes according to http://www.ahrq.gov/research/sep04/0904RA4.htm, though it is not as cost effective.