
![]()
Dexamethasone
The new treatment for Covid-19
![]()
![]()
Molecule of the Month July 2020
Also available: HTML version.
![]()
 |
DexamethasoneThe new treatment for Covid-19
Molecule of the Month July 2020
|
 |
Not quite, but it is the first real treatment that’s been shown to be effective against COVID. In June 2020 a UK trial showed that it can save the lives of up to a third of patients who are on a ventilator as a result of COVID-19. And it could save the lives of one in five of those patients receiving oxygen.
It doesn’t really help them – it’s really only of benefit to the sickest patients.
Dexamethasone is an odourless white to off-white crystalline powder, with a slightly bitter taste, that is a derivative of cortisone.
I’ve heard of cortisone – that’s the ‘stress hormone’!Yes, that’s correct. Cortisone is one of the main hormones released by the adrenal gland in response to stress. More precisely, this, and other similar hormones, are made in the ‘adrenal cortex’ (the outer layers of the gland) – hence the name cortisone. Cortisone is the ketone version of the alcohol cortisol (which is also known as hydrocortisone when it's used as a medicine), which is another steroid released by the adrenal gland. Biochemical reactions in the body can readily covert cortisone into cortisol and back again, so the two names are often used interchangeably. What do you mean by 'stress'?'Stress' can mean many things, but medically it often refers to an injury or infection that causes the body’s defences and immune response to kick in. Cortisone’s main function is to suppress the immune system, thus reducing inflammation and attendant pain and swelling at the site of the injury. Why would you want to suppress the immune system – surely you want to repair the injury?It depends on the timescale. In the short term, it might be more important to escape from immediate danger (e.g. an attacking lion) than to slow down and repair wounds. Cortisone works together with adrenaline (see MOTM from May 1999) to give the animal (or human) the ability to fight-or-flight, without having to deal with pain or swellings. Once the animal is safely out of harm’s way, the cortisone level subsides, and the repair and immune systems get to work protecting and repairing the injury. |
 Image: Phee / CC BY-SA from Wikimedia Commons |
One of the reasons you may have heard of cortisone is that it’s linked to early death from illness or heart attacks. People that suffer from prolonged stressful situations, due to pressure of work or home life, continuously release cortisone into their bloodstreams. This lowers their immune response and makes their body much more susceptible to illness or disease and less able to repair damage.
Cortisone was discovered in 1925 by American chemists Edward Calvin Kendall and Harold Mason while working at the Mayo Clinic in the USA. A few years later, Philip Hench discovered that cortisone was effective in the treatment of rheumatoid arthritis. This led to Kendal, Hench and a Swiss chemist called Tadeusz Reichstein, being awarded the Nobel prize for medicine in 1950.
 |
 |
 |
| Edward Calvin Kendall | Philip Hench | Tadeusz Reichstein |
Nowadays cortisone is used to treat a variety of ailments either in form of a pill or injections. Many people will know about cortisone injections being used to give short-term pain relief and reduce the swelling from inflammation in the knee or elbow joints, particularly after sports injuries (such as ‘tennis elbow’). Cortisone may also be used to deliberately suppress the immune response in patients with autoimmune diseases (such as arthritis) or to prevent rejection following an organ transplant. Some skin ailments like eczema and dermatitis can often be helped by suppression of the immune system using cortisone.
However, there are some problems and side-effects associated with the long-term use of cortisone. So, from the early 1950's, chemists began modifying its structure in the hope of improving its performance and eradicating the side-effects. Such synthetic modified structures are known as ‘corticosteroids’.
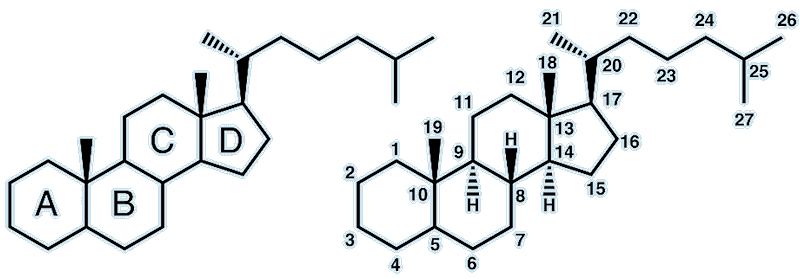
Steroids are molecules that contain three six-membered rings and one 5-membered ring fused together, attached to a carbon side-chain. They have a number of important biochemical roles, such as hormones like testosterone and estradiol and lipids such as cholesterol. The rings are labelled A, B, C and D, while the carbons are numbered consecutively starting from the top carbon in ring A.
[Image: Boghog2 / Public domain
From trials with rats, it was found that cortisone was rapidly reacting with chemicals in the body rendering it inactive, meaning the dosage had to be increased or the drug adminstered continuously to have the desired effect. The chemical reaction attacked the side-chain, so to prevent this, a group of chemists led by Glen Arth working at the Merck, Sharp & Dohme Laboratories Divison in Rahway, New Jersey, added a methyl group at carbon-16 in the steroid ring (shown in red in the structure, below). This stabilised the side-chain and increased the lifetime and effectiveness of the new drug.
 |
 |
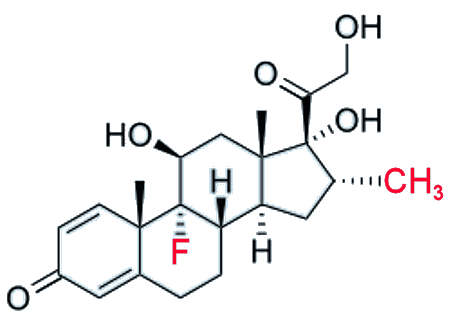 |
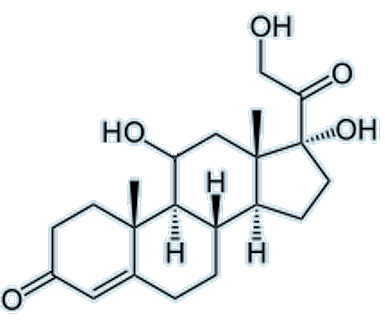
| Cortisol The difference between this and cortisone is the OH group at C-11. |
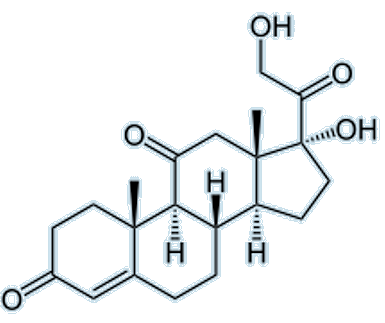
Cortisone The OH group at C-11 has now been converted into a ketone, C=O. |
Dexamethasone The methyl group at C-16 and the F at C-9 are shown in red. |
Not quite. A range of so-called ‘16-methylated steroids’ was produced all with slightly modified structures, but there was still a problem; usage of these drugs caused excessive retention of salt, and by extension, water. Thus, bloating could occur, and swellings would not reduce as quickly as needed. A group of chemists led by Joseph Bunum working at the National Institute of Arthritis and Metabolic Diseases in Bethesda, USA, tried to solve this by, again, further modifying the structure. They discovered that adding halogen atoms on the carbon-9 position reduced salt retention. After testing many different structures on rats, they found one of these new molecules that contained a fluorine group at C9 (also shown in red, above) was “the most potent of any steroid heretofore studied”.
The new drug, named dexamethasone, was approved for medical use in 1961, and is now widely prescribed for a host of common ailments, including skin diseases, severe allergies, asthma, croup, and many inflammatory and autoimmune conditions, such as rheumatoid arthritis. It is sometimes given in small amounts by dentists before and/or after the extraction of wisdom teeth to reduce cheek swelling. It is also given to some cancer patients to counter the inflammation that can occur with certain forms of chemotherapy. Mountain climbers often carry dexamethasone because it can help deal with the complications of high-altitude sickness.
There are always side-effects with any medicine. Dexamethasone may cause anxiety, difficulty sleeping, weight gain and fluid retention. But these are rare and usually associated with prolonged high dosages.
 So what about COVID-19?
So what about COVID-19?The fact that it is a cheap, commonly available drug that has been around for 50 years and has been thoroughly tested, means that it could be crucial in the fight against COVID-19. Because it is used to treat so many common ailments, most countries have a large stock of it. And because it's been around for such a long time, the patent has expired, which means many companies around the word can make the drug freely. In the UK it costs around £5 a dose, with around 10 doses required for COVID treatment. In India and many African counties it’s even cheaper, costing less than two dollars a dose.
The results come from the Recovery (Randomised Evaluation of COVID-19 therapy) trial conducted by the University of Oxford in June 2020 where 2,100 patients received a 6 mg daily dose of dexamethasone for 10 days. Their progress was compared with a random control group of ~4,300 patients who received no additional treatment. Results suggest that for every 100 COVID patients on a ventilator for 28 days, 60 are likely to recover anyway, 28 will die anyway even with the new drug, but 12 patients (who otherwise would die) will now survive due to dexamethasone.
Although this result has not yet been published or peer-reviewed, the outlook is very promising. And just as before, there are a range of corticosteroids with slightly different structures that are currently being studied in case they are even more effective at treating severe COVID patients.
![]()
![]()
![]() Back to Molecule of the Month page. [DOI:10.6084/m9.figshare.12510626]
Back to Molecule of the Month page. [DOI:10.6084/m9.figshare.12510626]