 |
Born again withIbogaine? |
 |
Born again withIbogaine? |
![]()
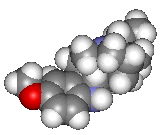
Also available: HTML-only, VRML and Jmol versions.
![]()
There is not much in the plant world that people have not sniffed, snorted, smoked, rubbed in, injected or attempted to get inside their bodies in other ways in the hope of eliciting someone kind of magical response. The well-known plants that gave a positive result in the primitive tests - the coca plant, poppies, marijuana, tobacco, betel trees, coffee beans - have since grown infamous leaving the air heavy with their tragic scent in so many places.
 If plants are our downfall, then they might also be our salvation. An African shrub - Tabernanthe iboga (right) - related to the coffee plant, offers some kind of hope for those who are addicted to alkaloid charms. Iboga has, like countless other herbal products, been used in traditional ceremonies and medicine for hundreds, if not thousands of years. In particular, in tropical West Africa it is a well-known hallucinogen used in male rites of passage but also as a tool by hunter to increase awareness and allow them to remain very still for prolonged periods. The physiologically active
compound is an indole alkaloid called ibogaine*. Surprisingly though, ibogaine is not itself addictive and even more intriguing is that it seems to have anti-addictive qualities. Take this drug and it cures addiction to another.
If plants are our downfall, then they might also be our salvation. An African shrub - Tabernanthe iboga (right) - related to the coffee plant, offers some kind of hope for those who are addicted to alkaloid charms. Iboga has, like countless other herbal products, been used in traditional ceremonies and medicine for hundreds, if not thousands of years. In particular, in tropical West Africa it is a well-known hallucinogen used in male rites of passage but also as a tool by hunter to increase awareness and allow them to remain very still for prolonged periods. The physiologically active
compound is an indole alkaloid called ibogaine*. Surprisingly though, ibogaine is not itself addictive and even more intriguing is that it seems to have anti-addictive qualities. Take this drug and it cures addiction to another.
The main claim made by advocates of ibogaine for treating drug addiction is that one dose is generally enough. With ibogaine, there is no need for weeks and weeks of regular methadone to stave off the chilling withdrawal symptoms of heroin, nor the increasing possibility of addiction to the treatment itself emerging. The fear of the detoxification process is claimed by drug rehabilitation centres to be the major obstacle to most addicts beating their habit. One dose - or at the most intermittent doses for two years - can it is claimed remove the destructive addiction of several hard drugs - cocaine and heroin, for instance - but even alcohol and nicotine. It is especially effective in those who actually want to give up.
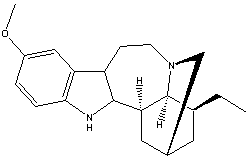 Ibogaine |
Howard Lotsof (below) is the man who holds the patents on using ibogaine to treat cocaine dependence, opiate addiction and multiple drug addiction disorders. He has championed its use in treating drug addiction for thirty years having experimented with it as a heroin addict himself in the 1960s. Basically, he and friends looking for a new high tried the drug and discovered after a rather prolonged hallucinogenic experience that their craving for heroin had simply vanished - or at least that's what he reports. Lotsof began years later - having succumbed to heroin again and having followed a full detoxification treatment - that there might be money to be made in this heroin cure.
 The product he hopes to market goes by the rather obvious name Endabuse and is causing a stink in the US law courts. The Federal Drug Administration and National Institute for Drug Addiction will soon be locked in battle with a neurologist studying the drug and Lotsof's company NDA International.
The product he hopes to market goes by the rather obvious name Endabuse and is causing a stink in the US law courts. The Federal Drug Administration and National Institute for Drug Addiction will soon be locked in battle with a neurologist studying the drug and Lotsof's company NDA International.
NDA International convinced several researchers to take a close look at ibogaine's effects on opiates several years ago. One of the scientists Stanley Glick, at Albany Medical College found that in lab rats treated with ibogaine before a morphine injection, the release of the neurotransmitter dopamine was partially blocked. (Dopamine is thought to be responsible for reinforcing the pleasurable effects of drugs of abuse.) Glick also discovered that following ibogaine injection, rats with free access to morphine cut down on their intake and had less withdrawal symptoms.
No definitive mode of action of ibogaine's supposed anti-addiction properties has yet been described. The molecular basis for addiction itself is not understood so this is unsurprising. However, ibogaine is known to be antagonistic to N-methyl-D-aspartate (NMDA) receptors. These receptors are thought to mediate some of the acute effects of drugs of abuse but by blocking them one may block the development of compulsive drug seek and taking. Ibogaine also seems to have activity in many neurotransmitter systems including serotonin uptake sites and sigma sites. It might be that its complexity of action has something to do with its activity. To confuse the picture still further there is also a putative long-lasting metabolite, O-desmethylibogaine which has not been investigated closely yet. However, according to Piotr Popik a psychopharmacologist at the Institute of Pharmacology, Polish Academy of Sciences, Krak�w, working mainly on the mode of action of "anti-addictive" drugs, The NMDA antagonistic actions are enough to explain most of the 'anti-addictive' effects of ibogaine.'
Not all scientists are convinced of the healing properties of those suffering addiction. Among ibogaine's side-effects are ataxia (loss of muscle coordination), nausea, vomiting and raised blood pressure. The compound also causes tremors, hallucinations and apprehension. Moreover, there is still the death to consider in the cancelled FDA trials.
 |
Could ibogaine stop the addiction to deadly drugs such as heroin? |
Popik is somewhat sceptical of ibogaine's potential. Popik co-authored the review with Glick. He points out that ibogaine is not in fact unique, 'All of the known antagonists of the NMDA receptor produce 'anti-addictive' effects in animal models of compulsive drug seeking and taking.' A simple test he and his colleagues carried out demonstrated that ibogaine is indeed an NMDA antagonist but the fact is there are countless other less harmful compounds with this same activity. Ibogaine produces a lot of neuropathological changes in the cerebellum, Popik adds. 'Briefly: I would not give it to my mother!' he told Catalyst. Meanwhile, Glick's team at Albany Medical College has developed a synthetic iboga alkaloid 18-methoxycoronaridine (18-MC). Their animal tests show that 18-MC has similar activity to ibogaine but may not have ibogaine's hallucinogenic properties.
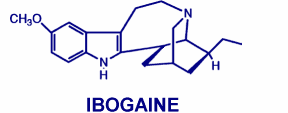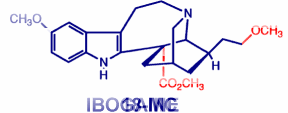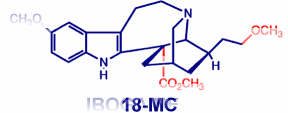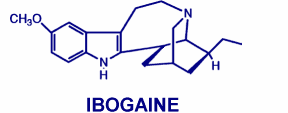 |
|
| The differences between 18-MC and Ibogaine. (taken from http://www.amc.edu/academic/Research/cnnResearcher.cfm?ID=130) | 18-MC |
The extraction of ibogaine from the roots and bark of Tabernanthe were first described in JACS in 1958 and its synthesis again in JACS in 1966, these classic recipes have quickly found their way out of the student locker and into Internet folklore, just as have methods for making fireworks and LSD. Aside from growing interest sparked by the Internet, ibogaine does not seem to have made its way on to the streets. Drug-pushers are perhaps wary of selling something that could cut their markets for other drugs in one fell swoop.
Something is also keeping ibogaine from the medical mainstream. Could it be that the authorities believe the existence an anti-addictive would actually increase drug abuse as users would experiment keenly, knowing that a quick and easy escape route was available to them. With the UK government revealing results of research that show heroin use is spreading out from the inner cities and into the shires, and the Home Office predicting an epidemic of addiction, it is perhaps time to take a closer look at the weapons we use to wage the war on drugs.
![]()
* For those who cannot resist a bit of nomenclature here is ibogaine: 7-Ethyl-6,2,7,8,9,10,12,13-octahydro-2-methoxy-6,9-methano 5H-pyrido(1',2':1,2- azepine(4,5-)indole. It also goes by the name of NIH 10567 and Endabuse.
The first report of the putative anti-addictive properties: Dzoljic ED, Kaplan CD, Dzoljic MR, Effects of Ibogaine on Naloxone-Precipitated Withdrawal Syndrome in Chronic Morphine- Dependent Rats, Archive of International Pharmacodynamics, 1988, 294, 64-70.
The Ibogaine Dossier - many links from here about Ibogaine.
Further reading: P. Popik and P. Skolnick, 'Pharmacology of Ibogaine and Ibogaine-Related Alkaloids', The Alkaloids, Academic Press, 1998, pp. 197-231.
This article originally appeared in The Alchemist on ChemWeb.com
![]()
![]() Back to the Molecule of the Month page
Back to the Molecule of the Month page