 |
ARTEMISININThe new antimalarial drug from China
Simon Cotton
Also available: HTML version.
|  |
 |
ARTEMISININThe new antimalarial drug from China
Simon Cotton
Also available: HTML version.
|  |
Yes, that's right.
Something like 200 million people are infected with malaria each year, and over a million will die, mainly children aged under five, in sub-Saharan Africa. New treatments are badly needed.
 Aren't there other drugs for treating malaria?
Aren't there other drugs for treating malaria?Until the 1930s, quinine was the antimalarial drug of choice. After war broke out in the Pacific at the end of 1941, the Dutch quinine plantations in the East Indies became inaccessible, and synthetic alternatives like chloroquine (see MOTM page on quinine) came into use. These drugs were successful for some years, but after a while the Plasmodium falciparium and Plasmodium vivax parasites developed resistance to chloroquine and other antimalarial drugs, meaning that new treatments were needed.
Not all the parasites are the same. Some will possess genetic differences that make them resistant to a particular drug molecule, which can be passed on to their offspring.
For the past century, all the alternative treatments for malaria have been synthetic drugs. Artemisinin was discovered due to the Vietnam war. Because there were many casualties in the North Vietnamese army, Ho Chi Minh, the North Vietnamese leader, got in touch with Zhou en Lai, the Premier of the Chinese Republic, as North Vietnam had China's backing. Possibly because Zhou en Lai himself had experienced malaria some 40 years earlier, the Chinese leadership swung into action, setting up a secret military project, known as 'Project 523' from the date on which the programme was launched, the 23rd day of the fifth month in 1967.
 So they invented a new drug?
So they invented a new drug?Not quite, they reinvestigated an old one, by looking at a 2000-year-old Chinese pharmacopoeia, Ge Hong's 'The Handbook of Prescriptions for Emergency Treatments'. This identified qinghaosu, obtained from sweet wormwood (Artemesia annua) (photo, right) as a remedy for fevers. They tried extracting the herb with hot solvents, but success only followed when they realised that the ancient text ran "Soak a handful of qinghao in water, wring out the juice and drink it all", so they tried extraction with cold ether, which worked. Animal tests were a success, then the team tried it on themselves before it went into clinical trials, where it was found to be better than chloroquine. Artemisinin itself, the active molecule, was isolated in 1972. When its structure was determined in 1975, it was found that its activity stemmed from a novel endoperoxide bridge. For some years artemisinin was not known in the West, until it was revealed at a conference in 1981.
 Who was responsible for the discovery?
Who was responsible for the discovery?A lot of scientists were involved. The two main protegonists are reported to be Zhenwing Wei and Youyou Tu (photo, left). In 2011 the latter received the prestigious Lasker award in clinical sciences for her work.
At just the moment that the malaria parasites were becoming resistant to all the existing drugs.
How does artemisinin work?At first it was thought that the peroxide group combined with iron in infected red blood cells and generated very reactive free radicals that destroyed key molecules and led to the death of the parasite - a kind of "dirty bomb". However, in 2003, a research team headed by Dr Sanjeer Krishna at St George's Hospital Medical School in London discovered that artemisinin inhibited an enzyme called Plasmodium falciparium ATP6 (PfATP6) responsible for a "pump" transporting calcium ions across cell walls in the parasite, though it seems that both iron and the peroxide group are important to its action. |
|
Unfortunately, no. Increasingly, people are worrying about the possibility of the malaria parasite becoming resistant to artemisinin. In 2005, researchers found that a mutation of one amino acid meant that the parasite became resistant. The World Health Organisation is now pressing for artemisinin to be used only in combination with another drug. They are urging the adoption of ACT (Artemisinin Combination Therapy) in which artemisinin is mixed with another drug like mefloquine, the thinking being that whilst a particular parasite might be resistant to one of the drugs, it is exceedingly unlikely to be resistant to two or three of them, so drug-resistant parasites will be eliminated. At the moment, approved combination therapies involve artemether or artesunate in particular. These and some other derivatives have better medicinal properties than artemisinin.
 |
 |
 |
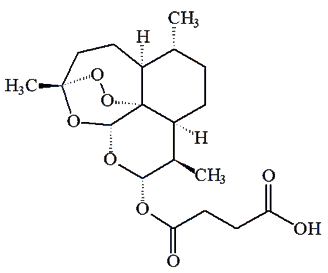
Artesunate |
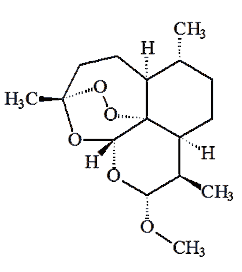
Artemether |
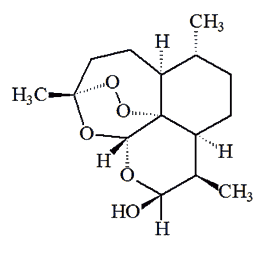
Dihydroartimisinin |
Although artemisinin itself has drawbacks as a medication (e.g. weak oral activity, poor solubility either in oil or water) it is readily reduced by NaBH4 to dihydroartemisinin, which in turn is readily converted into useful derivatives like artemether and artesunate.
 Another problem with artemisinin is simply due to its success. It is in very short supply and is also relatively expensive. Artemisinin is largely obtained from sweet wormwood, which contains less than 1% artemisinin. Making artemisinin from scratch ("total synthesis") requires many steps, and is also expensive. Two promising routes have been described; one uses "engineered" yeast (Saccharomyces cerevisiae) to produce artemisinic acid, via farnesyl pyrophosphate, and amorpha-4,11-diene. Others have reported a single continuous-flow process that makes artemisinin from dihydroartemisinic acid, itself easily made from artemisinic acid. It is possible that these processes could be scaled up to produce artemisinin industrially in large quantities, thereby reducing the cost of ACT to a level where it could be afforded by Third World economies.
Another problem with artemisinin is simply due to its success. It is in very short supply and is also relatively expensive. Artemisinin is largely obtained from sweet wormwood, which contains less than 1% artemisinin. Making artemisinin from scratch ("total synthesis") requires many steps, and is also expensive. Two promising routes have been described; one uses "engineered" yeast (Saccharomyces cerevisiae) to produce artemisinic acid, via farnesyl pyrophosphate, and amorpha-4,11-diene. Others have reported a single continuous-flow process that makes artemisinin from dihydroartemisinic acid, itself easily made from artemisinic acid. It is possible that these processes could be scaled up to produce artemisinin industrially in large quantities, thereby reducing the cost of ACT to a level where it could be afforded by Third World economies.
 |
 |
 |
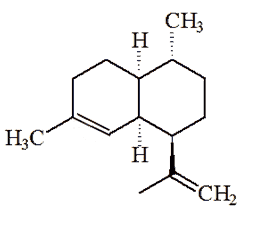
Amorpha-4,11-diene |
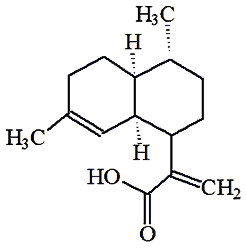
Artemisinic acid |
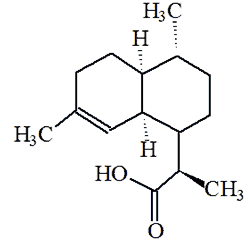
Dihydroartemisinic acid |
Another artemisinin-type molecule known as artemisone was reported in 2006. It combines high activity against the malarial parasite with other desirable features including low lipophilicity (solubility in fat) and negligible neuro- and cytotoxicity (i.e. it's not poisonous to either cells or the nervous system).
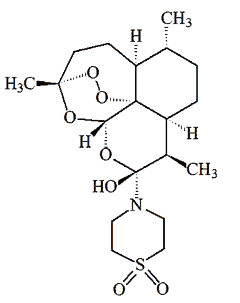
Artimisone
Yes, but maybe not for good. Scientists have synthesised molecules containing one or two peroxide bridges. Some of these are so new they haven't been given proper names yet, and just have code names. These include OZ277, OZ439 and RKA 182, and they are currently being tested to see how effective they are.
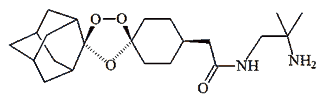 |
OZ277 |
|
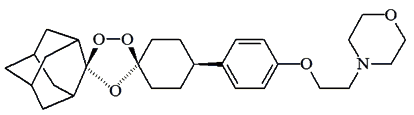 |
OZ439 |
|
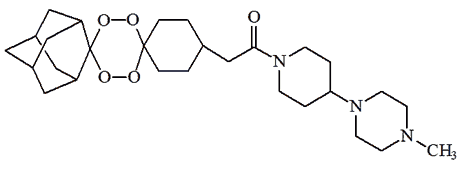 |
RKA182 |
![]()
![]()