![]()
FOLIC ACID
A necessary ingredient
for building DNA, cells and babies
![]()
Dominic Taylor and Paul May
University of Bristol, Bristol, UK
![]()
Molecule of the Month August 2008
Also available: HTML ersions.
![]()
 |
FOLIC ACIDA necessary ingredient
|
 Folic acid (vitamin B9) is important in a number of human metabolic pathways as well as being needed for nucleic acid synthesis, growth and the healthy development of a foetus [1]. Folic acid can be absorbed from the diet, with the highest levels of folic acid being found in foods such as meat extracts (e.g. Bovril), yeast extracts (e.g. Marmite), liver, asparagus, brussel sprouts, spinach, as well as being available as supplements [1]. Recently cereals and bread have been fortified with folic acid to try and eliminate folic acid deficiency especially in pregnant women.
Folic acid (vitamin B9) is important in a number of human metabolic pathways as well as being needed for nucleic acid synthesis, growth and the healthy development of a foetus [1]. Folic acid can be absorbed from the diet, with the highest levels of folic acid being found in foods such as meat extracts (e.g. Bovril), yeast extracts (e.g. Marmite), liver, asparagus, brussel sprouts, spinach, as well as being available as supplements [1]. Recently cereals and bread have been fortified with folic acid to try and eliminate folic acid deficiency especially in pregnant women.
 |
|
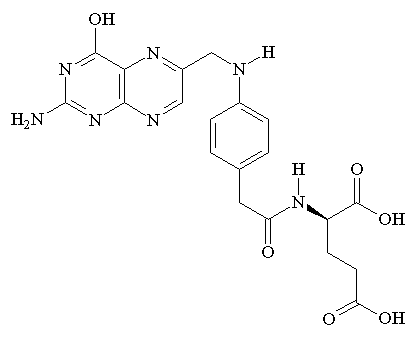
| Structure of folic acid |
Folic acid (pteroylglutamic acid) is composed of three large sub-components. These are the pteridine ring, para-amino benzoic acid, and glutamic acid. Glutamic acid is an amino acid that the body can actually synthesize by itself and is found in proteins. Folic acid gets its name from the Latin word folium meaning "leaf", since it's found in many leafy plants. This fully oxidized form is not found naturally but is what is used in supplements. Reduced polyglutamates are what are found in animal and plant foods (see below).
 The nutritional benefits of folic acid were first observed by researcher Lucy Wills (photo. left) in 1931 while she was researching anaemia in pregnant textile workers in Bombay, India. It was here that she discovered that treating these patients with yeast and liver extracts cured the anaemia [2]. This extract was called the 'Will's factor', but it wasn't until late in the 1930s that folates (compounds with the same vitamin activity including naturally occurring folates and folic acid) were discovered to be the active agent in the cure of anaemia. Folic acid was first isolated from spinach in 1941, and synthesised in pure crystalline form by Bob Stokstad in 1943 [3].
The nutritional benefits of folic acid were first observed by researcher Lucy Wills (photo. left) in 1931 while she was researching anaemia in pregnant textile workers in Bombay, India. It was here that she discovered that treating these patients with yeast and liver extracts cured the anaemia [2]. This extract was called the 'Will's factor', but it wasn't until late in the 1930s that folates (compounds with the same vitamin activity including naturally occurring folates and folic acid) were discovered to be the active agent in the cure of anaemia. Folic acid was first isolated from spinach in 1941, and synthesised in pure crystalline form by Bob Stokstad in 1943 [3].
 |
|
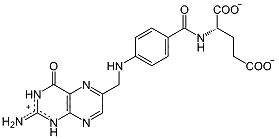
| 'Folates' in common usage means all pteroglutamates having vitamin activity, but the true folate ion is the one shown above. |
 It is now widely accepted that folic acid deficiency in the mother is a major cause of birth defects in the baby, especially neural tube defects (NTDs), the most common of these being spina bifida and anencephaly. Spina bifida is when the baby is born with an exposed spinal cord, and anencephaly is when the bone covering the cerebral cortex fails to develop [4,5]. The neural tube is the early spinal cord found in embryos which forms 28 days after conception. Because this is early in pregnancy, most NTDs develop before women realise they are pregnant - and therefore too late to do anything about it. There are a number of prenatal tests that are carried out during pregnancy to test for NTDs, which, if discovered, normally leads to termination of the pregnancy [5].
It is now widely accepted that folic acid deficiency in the mother is a major cause of birth defects in the baby, especially neural tube defects (NTDs), the most common of these being spina bifida and anencephaly. Spina bifida is when the baby is born with an exposed spinal cord, and anencephaly is when the bone covering the cerebral cortex fails to develop [4,5]. The neural tube is the early spinal cord found in embryos which forms 28 days after conception. Because this is early in pregnancy, most NTDs develop before women realise they are pregnant - and therefore too late to do anything about it. There are a number of prenatal tests that are carried out during pregnancy to test for NTDs, which, if discovered, normally leads to termination of the pregnancy [5].
The link between folate deficiency and NTDs was first suggested in 1964 by Brian Hibbard. Further research was carried by R.W. Smithells in 1983 while working as an obstetrician in Liverpool. Since then many other trials using folic acid supplements in pregnant women have been carried out all over the world, and have proven the link between folate deficiency and increased risk of NTDs [3].
Due to the early development of NTDs in foetuses it is important that women wanting to conceive should increase their folic acid intake before they conceive, as well as during the first 12 weeks of pregnancy. Since 1992 the US Public Health service has recommended that all women of child-bearing age should consume 0.4 mg per day of folic acid. Similarly, te NHS in the UK recommends that women wanting to become pregnant take supplements of 0.4 mg per day until the 12th week of pregnancy [6,7]. Research has shown that a daily supplement of 0.4 mg per day reduces the chance of NTDs by an estimated 36%, and in some cases 4 mg per day has been estimated to prevent 8 in 10 cases of NTDs, assuming the supplement was taken before pregnancy [8].
Even though the benefits of folic acid are well documented, the current daily intake of folic acid/folates among women aged 19-64 years is only 0.292 mg [9]. This is well below the recommended daily intake for pregnant women. Because the upper intake limit is as high as 1 mg per day, there is no reason why all women and men should not be reaching the 0.4 mg level.
 One of the ways to increase the folate intake in all people is through folic acid fortification of cereals and grains. There are different ideas on the levels of fortification and whether fortification should be mandatory or voluntary. For example in the USA, since 1998 all grains have been fortified with 0.14 mg/100 g of grain, and in Chile wheat flour has been fortified by 0.22 mg/100 g of grain - almost double the levels in the USA. In the USA this fortification has been estimated to increase a person's daily intake of folates by 0.1 mg per day [9], i.e. a quarter of the recommended daily dose.
One of the ways to increase the folate intake in all people is through folic acid fortification of cereals and grains. There are different ideas on the levels of fortification and whether fortification should be mandatory or voluntary. For example in the USA, since 1998 all grains have been fortified with 0.14 mg/100 g of grain, and in Chile wheat flour has been fortified by 0.22 mg/100 g of grain - almost double the levels in the USA. In the USA this fortification has been estimated to increase a person's daily intake of folates by 0.1 mg per day [9], i.e. a quarter of the recommended daily dose.
In the USA, since the implementation of mandatory fortification, the number of cases of NTDs fell from 37.8 per 100,000 live births before fortification, to 30.5. This is a decrease of 19%, which strongly supports the government's decision to make fortification mandatory. However, there are number of other factors, e.g. greater number of terminated pregnancies in which NTDs have been diagnosed, or increased use of folic acid supplements which could also contribute to the decrease [10]. Despite these facts, however, there are still groups opposed to mandatory folic acid fortification on the grounds of freedom of choice.
In the UK and many other EU countries, the debate on whether fortification should be mandatory continues. To date, no EU country has introduced mandatory fortification. Between 1995 and 1998 the UK Health Authority ran a folic acid campaign, aimed at increasing the awareness of the benefits of folic acid as well as increasing the availability of cereals and breads fortified with folic acid. The campaign was successful; in 2000 92% of mothers knew of the benefits of folic acid in early pregnancy compared with only 51% in 1995. Furthermore, 98% of mothers had increased their folic acid intake through supplements (73%) and changing their diet (31%) [11]. However, many commercial organisations argued they saw little benefit in voluntary fortification, because the target audience was too small to warrant serious investment and development.
Most recently, in 2007 the UK Food Standard Agency decided to recommend that folic acid fortification should be mandatory as part of an overall effort to increase folate levels in young women. They suggested that mandatory fortification of bread or flour will increase the levels of folate in around 13 million people in the UK who are currently folate deficient [12]. One advantage of folic acid fortification is that it is more effective at increasing folate levels in the body than naturally occurring folates found in food. This means eating foods fortified with folic acid have an advantage over eating foods naturally rich in folates [13].
 |
|
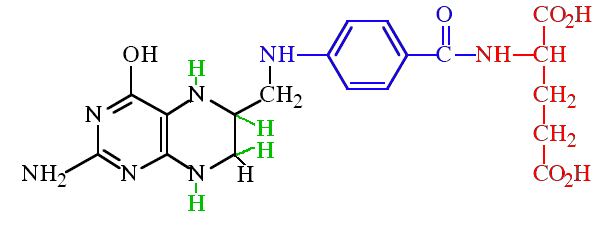
| Tetrahydrofolic acid. Folic acid is converted into dihydrofolic acid (DHFA) using various enzymes or coenzymes in the body, such as NADPH. This is then further converted to the tetrahydrofolate form (THFA, the 4 new H's are shown in green), which can then polymerise to form the various polyglutamates found in living organisms. |
![]() The hydrogenated ionic form of folic acid (THF, tetrahydrofolate) is used in the complex, enzyme-catalysed synthesis of DNA. It acts as a substrate to carry C1 groups (in the form of methanoate), and help in the biosynthesis of purines, serines and glycine - the building blocks of DNA.
The hydrogenated ionic form of folic acid (THF, tetrahydrofolate) is used in the complex, enzyme-catalysed synthesis of DNA. It acts as a substrate to carry C1 groups (in the form of methanoate), and help in the biosynthesis of purines, serines and glycine - the building blocks of DNA.
Unlike NTDs, the link between cancer and folic acid is still in its infancy. Folate deficiency is said to increase the chances of getting cancer of the brain, cervix, lung and colon. Folates play an important role in DNA synthesis and it has been hypothesised that a lack of folate will cause mutations and DNA strand breakage, leading to cancer [14]. On the other hand, there has been serious interest in a set of drugs known as antifolates, which are now being used as anti-cancer drugs. Because tumour cells replicate rapidly, a deficiency in folate would interrupt replication and reduce tumour growth [15].
Some studies have shown that the use of B vitamin supplements (including folic acid) have led to a decreased risk of cardiovascular diseases. The mechanism by which folic acid reduces the risk of CVD is unknown, but it has been linked with folic acid's ability to regulate hymocysteine [16,17]. Moderate-to-high levels of hymocysteine have been attributed to increased risk of coronary heart disease because of the negative effect hymocysteine has on blood vessels [17].
![]()
![]()