![]()
Vitamin B1 (Thiamine)
Deficiency of this causes beriberi
![]()
![]()
Molecule of the Month September 2017
Also available: JSMol version.
![]()
Vitamin B1 (Thiamine)Deficiency of this causes beriberi
Molecule of the Month September 2017
|
 |
No. It’s a disease that used to be common a hundred or more years ago, especially in South East Asia. The victims suffer weight loss, weakness, paralysis of the legs, swelling of arms and legs, and impaired nerve function. In later stages it can lead to mental confusion, brain damage and death. The term ‘beriberi’ is believed to originate from the Sinhalese (Sri Lankan) language, with the word ‘beri’ meaning either ‘weak’ or ‘I cannot’, which is duplicated for emphasis.
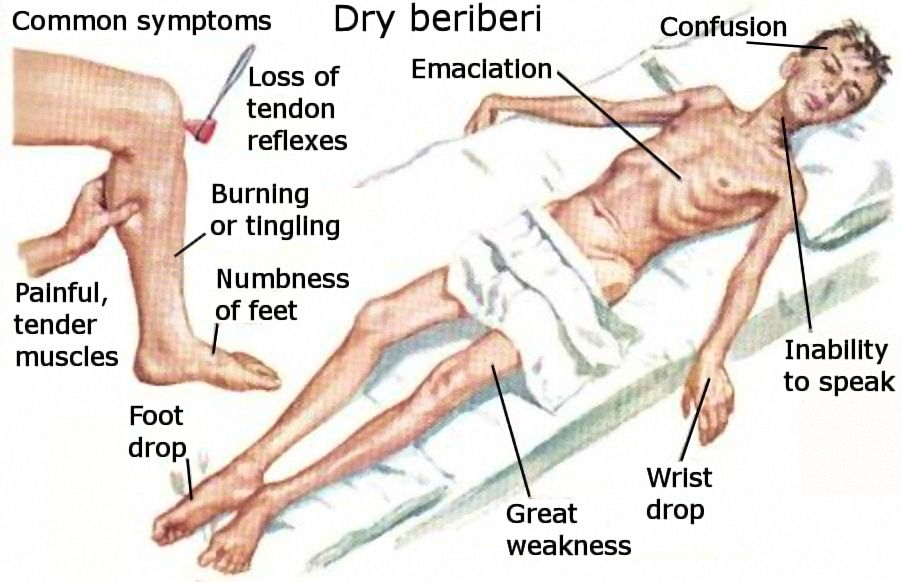
Some symptoms of ‘dry’ beriberi. There is also a ‘wet’ version of beriberi which mainly affects the heart and circulatory system,
with shortness of breath, swelling of the lower legs, and increased heart rate.
For many years this was a mystery. But there were some clues. First it was far more common in SE Asia than in Europe. Also, a number of intriguing reports seemed to suggest that in some places the poorer members of a village seemed to suffer less from beriberi than the wealthier members.
Yes, with most diseases the poor suffer the most. But this peculiarity did point to diet being involved. Further clues came when a Japanese medical doctor called Takaki Kanehiro was studying beriberi in the Japanese Navy. In the late 19th century, beriberi was a serious problem among Japanese sailors, especially on long voyages.
I thought scurvy was the sailor’s disease?In the west, that’s true. Scurvy, caused by a deficiency of vitamin C in the sailors’ diet, was a major killer of European sailors for hundreds of years (see MOTM July 2017 - Vitamin C), but in Far East navies, beriberi was more common. For example, in one particular incident studied by Kanehiro, of 376 Japanese sailing cadets on a 9-month training mission from Japan to Hawaii, 169 contracted beriberi and 25 died. Kanehiro had long suspected that diet was the key to curing beriberi, but this conflicted with the accepted theory that it was an infectious disease. So to prove it, he arranged with the Japanese Navy to send another ship along the same route as the previous ship, except that this new crew were fed a varied diet of meat, fish, barley, rice and beans, whereas the previous crew had had only standard rations consisting mostly of rice. The new better-fed crew only suffered 14 minor cases of beriberi and had no deaths. In a later study, Kanehiro also noticed that beriberi was rife among the ordinary sailors, but not among the officers – and also that beriberi was rare in Western Navies. |
|
Kanehiro spotted that the low-ranking sailors were given free white rice to eat, and so ate little else but this, but the officers had a more varied diet - similar to that of the sailors in Western navies.
That might be the first thought. But the officers were eating the same rice, too – except they were eating other foods as well. So, it was eating nothing but white rice that was making the sailors sick. It also explained why beriberi was associated with Asia, where rice eating was the staple food.
Yes, this was a conundrum. The person that solved this discrepancy was Christiaan Eijkman, who was working as a physician in the Dutch East Indies (now Indonesia) in 1897. He noticed that in order to improve its flavour and shelf-life, rice was usually milled to remove the husks, bran and germ. It was often then further polished using an abrasive dust to remove any last traces of the kernels. This high quality polished rice was then sold to the wealthier people, whereas the poorer farmers often just ate the unpolished rice with its kernel and husk intact.
 |
 |
| Christiaan Eijkman (Copyright: Museum Boerhaave, free for publication). |
Frederick Hopkins (Copyright: Nobel Committee, public domain) |
Not immediately. The breakthrough came when he noticed that some of the chickens in his laboratory had suddenly started to walk jerkily, and seemed to have contracted the symptoms of beriberi. It turned out that their feed had recently been changed to polished white rice, so as to use up left-overs from military rations. When the chicken-feed was reverted back to the normal source of general varied kitchen scraps the chickens soon recovered. Eijkman now realised that white rice lacked some essential ingredient, without which the chickens, and people, would get beriberi. Unfortunately, ill heath prevented him continuing with this work, but this hypothesis was later confirmed by his colleague Adolphe Vorderman using studies of the diets of prison inmates. By doing careful experiments with different foods and different sets of inmates (without them being told what the nature of the experiment was), he showed that the ‘anti-beriberi’ ingredient was in the husks and kernels of the rice. Between 1906 and 1912, the English biochemist Frederick G. Hopkins published detailed follow-up studies and confirmed the preliminary findings of Eijkman and Vorderman. For these discoveries, Eijkman and Hopkins shared the Nobel Prize for Medicine in 1929, although, rather unfairly, Vorderman’s contribution wasn’t acknowledged.

Unpolished brown rice (right) is the whole grain of rice with just the outer cover (the husk) removed.
Milled rice (centre) has the germ and bran layer removed.
Finally, polished white rice (left) is polished to a smooth finish, but what’s left is mostly starch.
Did Kanehiro get any recognition for his work?The Japanese Navy took him seriously, but unfortunately his findings were ignored by the Imperial Japanese Army, which continued to insist beriberi was an infectious disease, and did nothing to change the diet of its soldiers. In the Japanese war against Russia in 1904-5, over 200,000 soldiers got beriberi, and 27,000 of them died. This compared to 47,000 deaths from combat. Nevertheless, in 1905 Kanehiro was made a baron as a reward for his contribution in eliminating beriberi from the Japanese Navy, and was nicknamed the ‘Barley Baron’ after his suggestion that sailors should eat brown barley to prevent beriberi. He was also honoured after his death by having the Takaki Promontory named after him in Antarctica – the only peninsula in Antarctica named after a Japanese person. So what is it in rice husks that prevents beriberi?This was discovered in 1912 by a Polish biochemist called Casimir Funk, who isolated it from brown rice. He described it as the ‘anti beri-beri factor’, and called it ‘vitamine’, meaning an amine vital for life. He also postulated that there may be a number of other ‘vitamines’ necessary to prevent diseases such as scurvy [see MOTM for July 2017 - Vitamin C], rickets (MOTM for November 2015 - Vitamin D), etc., and published a book called The Vitamines in 1912. Although this idea was proved correct, it was later found that not all vitamins were amines, so the ‘e’ suffix was dropped. The anti-beriberi compound was named thiamine, meaning sulfur-containing amine. Vitamin A (MOTM Jan 2017) had already been discovered and named, so thiamine was a candidate to be called vitamin B. But because there were a host of other recently discovered water-soluble essential nutrients all vying to be called vitamin B, this category was subdivided into B1, B2, B3, etc., and thiamine was called vitamin B1. |
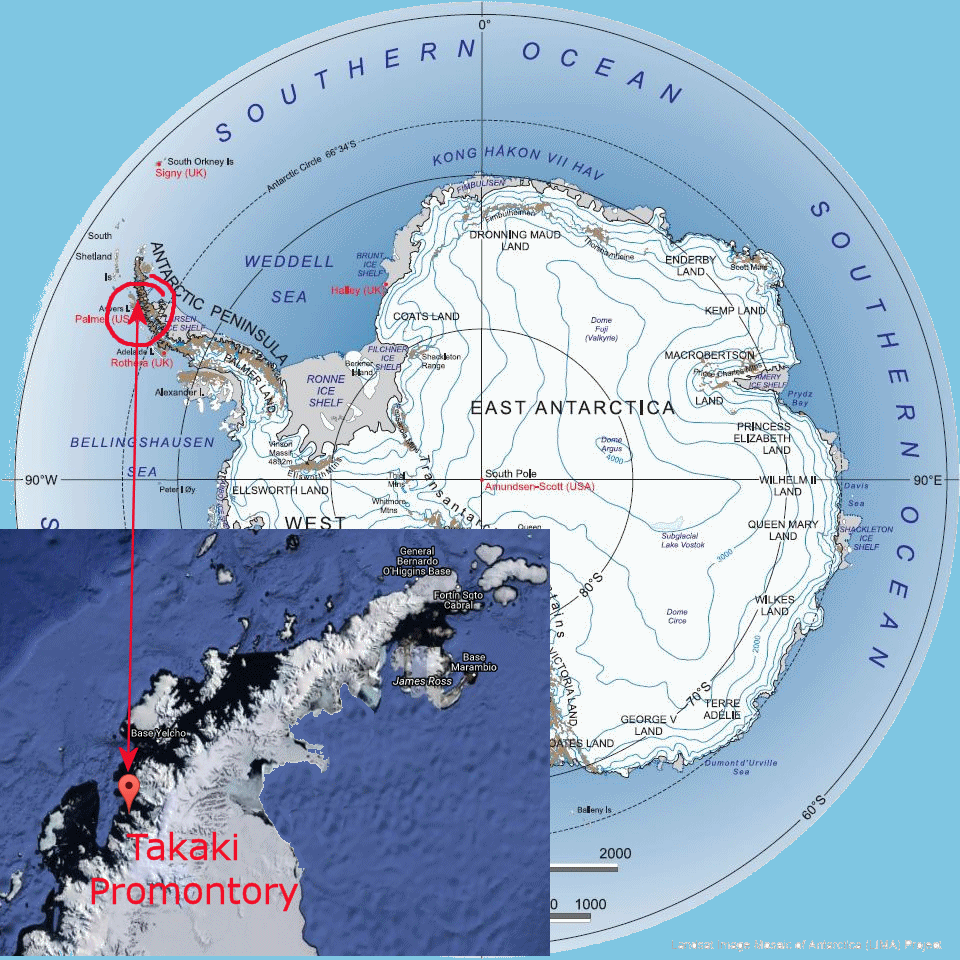 The location of the Takaki Promontory in Antactica. |
Chemically, thiamine is an aminopyrimidine ring linked to a thiazole ring by a methylene bridge. Humans cannot biosynthesise it, so it must be eaten in foods. It is found in a wide variety of foodstuffs, including seeds, beans, pork, spinach, cornflour, and breakfast cereals. Nowadays thiamine is added to many basic foods, such as white rice and flour, to prevent deficiencies. In the United States, people consume around half of their vitamin B1 intake in foods that naturally contain thiamine, while the rest comes from foods that are fortified with it. This means that beriberi is now very rare in people with modern diets, and is only really seen in areas of malnutrition, such as during famines, some prison camps (e.g. the notorious camps used by the Japanense to hold POWs during WW2), war zones, and in people who have diseases which prevent thiamine being absorbed efficiently, e.g. HIV or chronic alcoholism.
No, as usual, most people eating a normal diet won’t need supplements – and taking more vitamin B1 than you need won’t bring any extra health benefits and it will just get excreted in urine. However, taking supplements may help elderly people or pregnant women (or alcoholics).
It is a cofactor (a molecular helper) for a number of enzymes in the body which are responsible for the breaking down of sugars and carbohydrates that we eat in order to release energy for growth, nerve function and muscle tone. So it’s not surprising that a deficiency in vitamin B1 causes the symptoms of beriberi, i.e. it lowers energy levels, affects the nerves, and causes muscle wastage.
In the body, thiamine is often converted to thiamine pyrophosphate, TPP, (a.k.a. diphosphate, ThDP) by the addition of 2 phosphate groups.
The chemical reactivity comes about because the acidic H on the thiazole ring is easily donated, due to the fact that the negatively charged carbanion that remains is partially stabilised by the positive charge on the nearby N. This oxidised form of the compound containing both a positive and negative charge is called an ylide, and is very reactive toward a number of biochemical species, including those in the Citric Acid Cycle used to make acetyl-CoA (MOTM for May 2007).
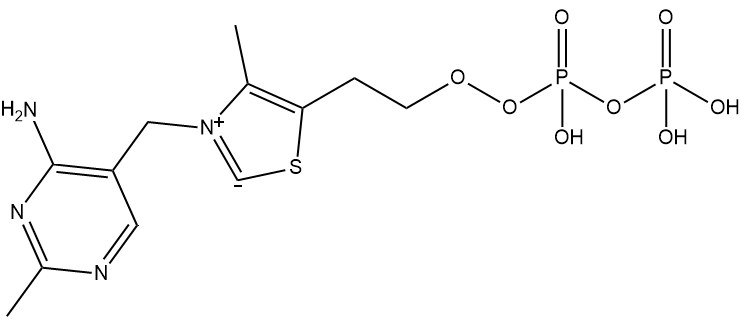
The ylide form of TPP
The main reaction it undergoes is a decarboxylation reaction, which means it splits a molecule apart at the C-C bond next to a carbonyl group, and removes the carbonyl as CO2. As part of the Citric Acid Cycle, the energy this reaction releases is eventually stored by linking phosphate groups to adenosine to form adenosine triphosphate, ATP (MOTM January 1998). In another biochemical route, this reaction helps to build the myelin sheath around nerve cells. So you can see that disruption to either of these two vital mechanisms will be catastrophic for the person involved.
![]()
![]()
![]() Back to Molecule of the Month page. [DOI:10.6084/m9.figshare.5260066]
Back to Molecule of the Month page. [DOI:10.6084/m9.figshare.5260066]